PZJuly working place
Saturday, February 27, 2021
Electromagnetic Waves - ppt video online download
Electromagnetic Waves - ppt video online download: Electromagnetic Theory Theoretical understanding Well developed by middle 1800’s Coulomb’s Law and Gauss’ Law explained electric fields and forces Ampère’s Law and Faraday’s Law explained magnetic fields and forces The laws were verified in many experiments
Tuesday, March 5, 2019
H.I.V. Is Reported Cured in a Second Patient, a Milestone in the Global AIDS Epidemic (nytimes)
Scientists have long tried to duplicate the procedure that led to the first permanent remission 12 years ago. With the so-called London patient, they seem to have succeeded.
By Apoorva Mandavilli
March 4, 2019
For just the second time since the global epidemic began, a patient appears to have been cured of infection with H.I.V., the virus that causes AIDS, scientists reported on Tuesday.
The news comes nearly 12 years to the day after the first patient known to be cured, a feat that researchers have long tried, and failed, to duplicate. The surprise success now confirms that a cure for H.I.V. infection is possible, if difficult, researchers said.
The investigators are to publish their report on Tuesday in the journal Nature and to present some of the details at the Conference on Retroviruses and Opportunistic Infections in Seattle.
Publicly, the scientists are describing the case as a long-term “remission.” In interviews, most experts are calling it a cure, with the caveat that it is hard to know how to define the word when there are only two known instances.
Both milestones resulted from bone-marrow transplants given to infected patients. But the transplants were intended to treat cancer in the patients, not H.I.V.
Bone-marrow transplantation is unlikely to be a realistic treatment option in the near future. Powerful drugs are now available to control H.I.V. infection, while the transplants are risky, with harsh side effects that can last for years.
But rearming the body with immune cells similarly modified to resist H.I.V. might well succeed as a practical treatment, experts said.
“This will inspire people that cure is not a dream,” said Dr. Annemarie Wensing, a virologist at the University Medical Center Utrecht in the Netherlands. “It’s reachable.”
Dr. Wensing is co-leader of IciStem, a consortium of European scientists studying stem cell transplants to treat H.I.V. infection. The consortium is supported by AMFAR, the American AIDS research organization.
The new patient has chosen to remain anonymous, and the scientists referred to him only as the “London patient.”
“I feel a sense of responsibility to help the doctors understand how it happened so they can develop the science,” he told The New York Times in an email.
Learning that he could be cured of both cancer and H.I.V. infection was “surreal” and “overwhelming,” he added. “I never thought that there would be a cure during my lifetime.”
At the same conference in 2007, a German doctor described the first such cure in the “Berlin patient,” later identified as Timothy Ray Brown, 52, who now lives in Palm Springs, Calif.
That news, displayed on a poster at the back of a conference room, initially gained little attention. Once it became clear that Mr. Brown was cured, scientists set out to duplicate his result with other cancer patients infected with H.I.V.
In case after case, the virus came roaring back, often around nine months after the patients stopped taking antiretroviral drugs, or else the patients died of cancer. The failures left scientists wondering whether Mr. Brown’s cure would remain a fluke.
Mr. Brown had had leukemia, and after chemotherapy failed to stop it, needed two bone-marrow transplants.
The transplants were from a donor with a mutation in a protein called CCR5, which rests on the surface of certain immune cells. H.I.V. uses the protein to enter those cells but cannot latch on to the mutated version.
Mr. Brown was given harsh immunosuppressive drugs of a kind that are no longer used, and suffered intense complications for months after the transplant. He was placed in an induced coma at one point and nearly died.

Timothy Ray Brown, the first person to be cured of H.I.V., almost died during the treatment.
Credit
Grant Hindsley for The New York Times
“He was really beaten up by the whole procedure,” said Dr. Steven Deeks, an AIDS expert at the University of California, San Francisco, who has treated Mr. Brown. “And so we’ve always wondered whether all that conditioning, a massive amount of destruction to his immune system, explained why Timothy was cured but no one else.”
The London patient has answered that question: A near-death experience is not required for the procedure to work.
He had Hodgkin’s lymphoma and received a bone-marrow transplant from a donor with the CCR5 mutation in May 2016. He, too, received immunosuppressive drugs, but the treatment was much less intense, in line with current standards for transplant patients.
He quit taking anti-H.I.V. drugs in September 2017, making him the first patient since Mr. Brown known to remain virus-free for more than a year after stopping.
“I think this does change the game a little bit,” said Dr. Ravindra Gupta, a virologist at University College London who presented the findings at the Seattle meeting. “Everybody believed after the Berlin patient that you needed to nearly die basically to cure H.I.V., but now maybe you don’t.”
Although the London patient was not as ill as Mr. Brown had been after the transplant, the procedure worked about as well: The transplant destroyed the cancer without harmful side effects. The transplanted immune cells, now resistant to H.I.V., seem to have fully replaced his vulnerable cells.
Most people with the H.I.V.-resistant mutation, called delta 32, are of Northern European descent. IciStem maintains a database of about 22,000 such donors.
So far, its scientists are tracking 38 H.I.V.-infected people who have received bone-marrow transplants, including six from donors without the mutation.
The London patient is 36 on this list. Another one, number 19 on the list and referred to as the “Düsseldorf patient,” has been off anti-H.I.V. drugs for four months. Details of that case will be presented at the Seattle conference later this week.
The consortium’s scientists have repeatedly analyzed the London patient’s blood for signs of the virus. They saw a weak indication of continued infection in one of 24 tests, but say this may be the result of contamination in the sample.
The most sensitive test did not find any circulating virus. Antibodies to H.I.V. were still present in his blood, but their levels declined over time, in a trajectory similar to that seen in Mr. Brown.
None of this guarantees that the London patient is forever out of the woods, but the similarities to Mr. Brown’s recovery offer reason for optimism, Dr. Gupta said.
“In a way, the only person to compare with directly is the Berlin patient,” he said. “That’s kind of the only standard we have at the moment.”

“I think this does change the game a little bit,” said Dr. Ravindra Gupta, a virologist at University College London.
Credit
Jane Stockdale for The New York Times
Most experts who know the details agree that the new case seems like a legitimate cure, but some are uncertain of its relevance for AIDS treatment overall.
“I’m not sure what this tells us,” said Dr. Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases. “It was done with Timothy Ray Brown, and now here’s another case — ok, so now what? Now where do we go with it?”
One possibility, said Dr. Deeks and others, is to develop gene-therapy approaches to knock out CCR5 on immune cells or their predecessor stem cells. Resistant to H.I.V. infection, these modified cells should eventually clear the body of the virus.
(CCR5 is the protein that He Jiankui, a scientist in China, claimed to have modified with gene editing in at least two children, in an attempt to make them resistant to H.I.V. — an experiment that set off international condemnation.)
Several companies are pursuing gene therapies but have not yet been successful. The modification must target the right number of cells, in the right place — only the bone marrow, for example, and not the brain— and tweak only the genes directing production of CCR5.
“There are a number of levels of precision that must be reached,” said Dr. Mike McCune, a senior adviser on global health to the Bill and Melinda Gates Foundation. “There are also concerns that you might do something untoward, and if so you might wish to have a kill switch.”
Several teams are working on all of these obstacles, Dr. McCune said. Eventually, they may be able to develop a viral delivery system that, when injected into the body, seeks out all CCR5 receptors and deletes them, or even a donor stem cell that is resistant to H.I.V. but could be given to any patient.
“These are dreams, right? Things on the drawing table,” Dr. McCune said. “These dreams are motivated by cases like this — it helps us to imagine what might be done in the future.”
One important caveat to any such approach is that the patient would still be vulnerable to a form of H.I.V. called X4, which employs a different protein, CXCR4, to enter cells.
“This is only going to work if someone has a virus that really only uses CCR5 for entry — and that’s actually probably about 50 percent of the people who are living with H.I.V., if not less,” said Dr. Timothy J. Henrich, an AIDS specialist at the University of California, San Francisco.
Even if a person harbors only a small number of X4 viruses, they may multiply in the absence of competition from their viral cousins. There is at least one reported case of an individual who got a transplant from a delta 32 donor but later rebounded with the X4 virus. (As a precaution against X4, Mr. Brown is taking a daily pill to prevent H.I.V. infection.)
Mr. Brown says he is hopeful that the London patient’s cure proves as durable as his own. “If something has happened once in medical science, it can happen again,” Mr. Brown said. “I’ve been waiting for company for a long time.”

A cake presented to Mr. Brown marking 12 years since he was cured, at a workshop at the Seattle Public Library on Sunday.
Credit
Grant Hindsley for The New York Times
Tuesday, February 26, 2019
《自然》子刊:肠道菌群与糖尿病关系实锤了!科学家发现肠道菌群分泌的丁酸会改善胰岛素响应,而丙酸会增加2型糖尿病风险丨临床大发现
https://mp.weixin.qq.com/s?__biz=MzA4MjA2MDI5OQ==&mid=2659483169&idx=1&sn=9a2bc5586541db77bc802fd096737c25&chksm=84fbab45b38c2253e077cfb7bf2e2ce575d07d8b5f4a37d1e29431af74d5a227ebfba980c3c4&mpshare=1&scene=24&srcid=0219B6B1OaQHlPVqMObAqItO#rd

本文通讯作者Cisca Wijmenga 博士
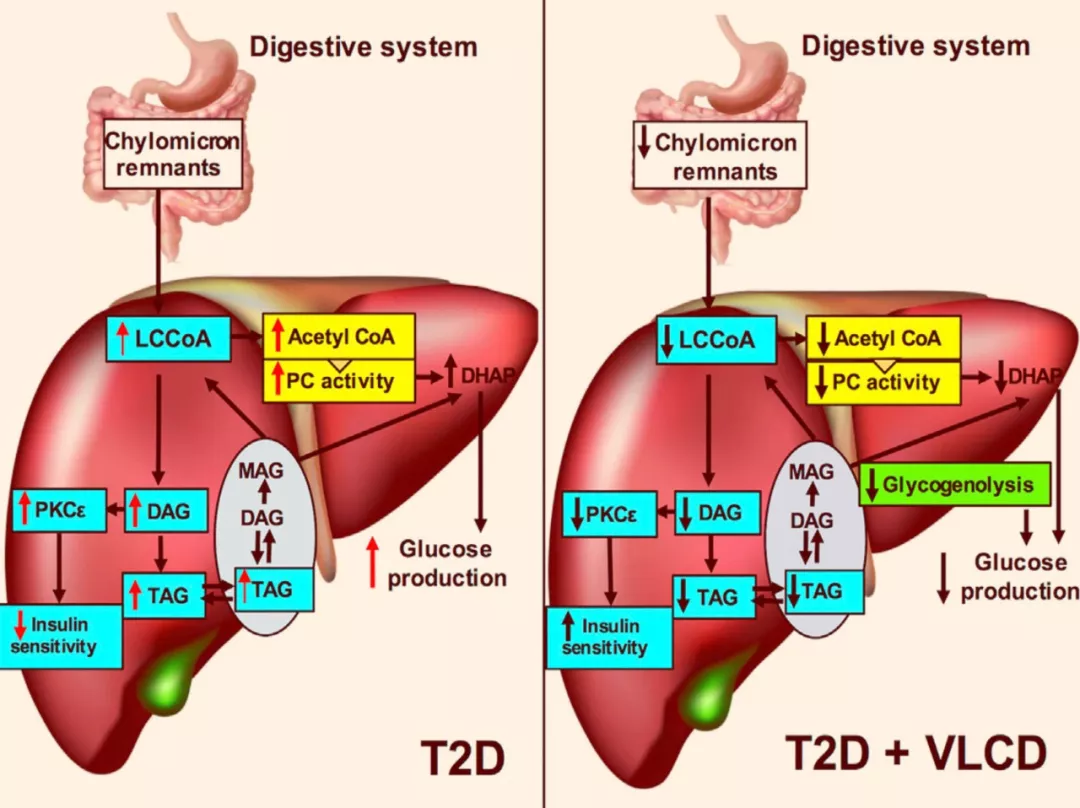
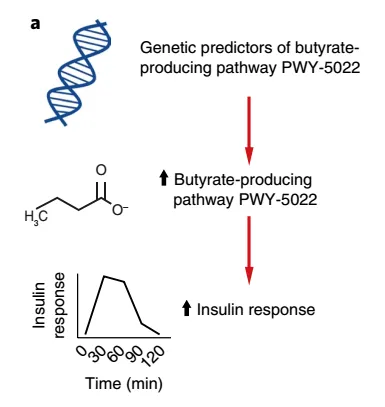
丁酸促进胰岛素响应
 瞬息瞬息万变,点击即达
瞬息瞬息万变,点击即达 小程序
小程序
这让奇点糕不尽感叹,人体到底谁说了算?!
不过,之前大部分研究都只是证明肠道微生物与疾病可能有关,并不能说明就是肠道微生物导致了这些疾病。
可是就在今天,科学家终于敲下了肠道微生物与一种常见疾病——糖尿病之间关系的实锤。
荷兰格罗宁根大学的Cisca Wijmenga 和英国牛津大学的Mark McCarthyl领导的一个联合团队发现,肠道微生物产生的丁酸,能改善人体的胰岛素响应;而另一种产物丙酸的异常,则会提高2型糖尿病的发病风险。相关研究发表在著名学术期刊Nature Genetics上[1]。
人体微生物的数量甚至超过了人体本身细胞的数量,如此庞大的菌群必然会对身体产生千丝万缕的影响。而大部分菌群又都存在于肠道中,因此,肠道微生物一直是近年来研究的热点。
不过,现在对肠道微生物的研究普遍存在一些问题。
一方面,很多研究都做的不够深入,很多情况下都只发现了一些相关性的证据(如菌群变动与疾病相关等),缺少细致的因果关系,这样就很难应用于临床[2]。
另一方面,还有不少研究是在动物身上完成的,例如,科学家就在动物中发现,肠道微生物促进2型糖尿病发展的原因[3]。这些研究可能找到因果关系,但很难说就一定适用于人体。
虽然人们发现,肠道菌群与2型糖尿病各种相关。可是目前还缺少在人体中,肠道微生物与2型糖尿病之间关系的直接证据。这也让通过干预肠道微生物,防止糖尿病的努力裹步不前。
不过,人们一直在努力朝这个目标前进。
之前有研究表明,由肠道微生物发酵产生的短链脂肪酸会影响血糖的水平[4]。但是,对于各种不同的短链脂肪酸(如乙酸、丙酸、丁酸等)到底发挥了怎样的作用,目前还不清楚。
为了搞清这个问题,研究者们收集了荷兰952名志愿者的数据,包括:全基因组数据、肠道宏基因组(指肠道中全部微生物的基因组)数据、粪便中短链脂肪酸的含量,以及他们的临床数据进行分析。其中,临床数据包括各种人体参数及血糖指标。
他们试图找到肠道微生物组——代谢产物组——人体指标(包括血糖指标)之间的具体联系。
从这些数据中,研究人员着重分析了245种微生物特征,包括2种粪便中的短链脂肪酸水平、57种独特的微生物分类单元以及186条微生物的信号通路。
他们通过一种叫双向孟德尔随机化设计的方法,来寻找微生物特征与血糖特征之间的因果关系。并用反变量加权方法进行检验,以鉴定出最佳的可能。
经过分析,研究人员发现在口服葡萄糖耐量试验中,4-氨基丁酸的降解与胰岛素分泌的上升有关。
4-氨基丁酸的降解产物正是丁酸。而在这些人的样本中,4-氨基丁酸降解通路活跃的菌(Eubacterium rectale和Roseburia intestinalis)正是著名的丁酸产生菌。
这说明丁酸很可能在摄入葡萄糖后,促进β细胞分泌胰岛素,调节血糖。
这个观点得到了一个独立的临床研究的证明。
一项对35名健康个体中的肠道菌群干预试验表明,通过补充益生菌降低产生丁酸盐的细菌的水平,会对葡萄糖代谢产生不利影响。
并且,研究人员还发现肠道菌群生产的另外一种短链脂肪酸——丙酸,会增加糖尿病的风险。粪便中丙酸含量越高,2型糖尿病风险越高。而对英国一个数据库里的数据进行检索,也印证了这个结果,粪便里丙酸水平升高与2型糖尿病的风险升高有关。
这说明丙酸可以作为预测2型糖尿病的风险因素。而且,人们可以从丙酸出发,寻找2型糖尿病产生的机制。
这个研究首次在人体中找到了,肠道菌群与胰岛素抵抗以及2型糖尿病之间的因果关系。即:丁酸可以促进餐后胰岛素分泌;而粪便中丙酸含量的增加,会提高2型糖尿病的风险。
当然,作者也表示,丙酸与糖尿病风险之间的因果关系,需要进一步的研究。现在还是要谨慎对待。
此外,虽然这个队列是目前在人群研究中最大的队列,但是仍然不足以弄清所有肠道微生物的特征。因此,后面需要更大、更全面的人群研究。
不过,无论如何,这个研究为后来的研究者们指明了方向。向人们展示了通过干预肠道微生物(如生产丁酸)治疗调节血糖,以及通过肠道微生物预测和及早防治2型糖尿病的广阔前景。
编辑神叨叨
丁酸在很多研究中(包括本研究)证明是一种有益的产物,不过也有报道称丁酸产量过高的话,也是有害的,因此要辩证地看。
未来是不是要研究下大脑微生物,看我们是不是真的被微生物控制的~
如果想及时获取第一手科研资讯,那你绝对不能错过瞬息~
参考资料:
[1] Serena Sanna et al. Causalrelationships among the gut microbiome, short-chain fatty acids and metabolicdiseases. Nature, 2019, Doi: org/10.1038/s41588-019-0350-x
[2] Brunkwall L, Orho-Me. 2 diabetes: fromcurrent human evidence to future possibilities[J]. Diabetologia, 2017, 60(6): 943-951.
[3] Kreznar J H, Keller M P, Traeger L L,et al. Host Genotype and Gut Microbiome Modulate Insulin Secretion andDiet-Induced Metabolic Phenotypes[J]. Cell Reports, 2017, 18(7): 1739-1750.
[4] Zhao L, Zhang F, Ding X, et al. Gutbacteria selectively promoted by dietary fibers alleviate type 2 diabetes[J].Science, 2018, 359(6380): 1151-1156.
刷新认知!含八种核苷酸的双链DNA首次问世,重新定义自然界遗传语言
https://mp.weixin.qq.com/s?__biz=MzA5NTYzMzAyNQ==&mid=2650191242&idx=1&sn=541fb1cc20046b2b966a94e9d51b8c0a&chksm=88be7e64bfc9f772d67b6a796de30703dd1de255a6d5b7adaab244b20207be511c35d0027704&mpshare=1&scene=24&srcid=0222jiANxPf3wmMe0ncnliwN#rd


图:IU SCHOOL OF OF MEDICINE
地球上的所有生命的遗传密码都基于四种核苷酸。而现在,科学家已经创造出了由八种核苷酸组成的双链DNA。
根据今日发表于《科学》杂志的一篇文章,研究人员通过将四种合成核苷酸与天然存在于核酸中的四种核苷酸相结合,突破性地创造了具有“八字母”的DNA分子结构,名为“Hachimoji(日语‘八’和‘字母’) DNA”。这是科学家首次创造出一种合成的“八字母”遗传语言,该分子结构和功能与天然的DNA分子相似,可以储存信息甚至被转录成RNA。研究人员表示,这种“八字母”DNA分子的信息存储能力是天然核酸的两倍,可能存在广阔的生物技术应用前景。此外,这一结果也扩大了可能支持生命的分子结构范围,包括整个宇宙的生命,表明了更广泛的化学物质可以支持生命。
在论文发表后,诸多业内资深人士也对这项成果表达了由衷的赞叹。
“这真是一篇激动人心的论文……一项杰出的技术成就。它如此优雅地增加了DNA及RNA构建模块的数量,并大大扩展了核酸的信息密度。”来自美国西北大学的生物工程学家Michael Jewett并未参与这项研究,但对这项成就赞叹不已。
来自斯克里普斯研究所的Floyd Romesberg对此评价道:“Steve现在所展示的是,你可以将DNA的单位翻倍,并保持可预测的化学过程,我认为这是惊人的,这是一项里程碑式的成就。”他还补充道,这项研究表明,在地球上进化出的四种化学物质并没有什么特别的“魔力”或特殊含义。 “这是一个概念上的突破。”
美国里士满大学生物学家Eugene Wu也表示:“看到有人设计出这样一个系统,真是令人兴奋。它引人思考这样一个生命起源的问题:为什么这4个核苷酸形成了核酸?为什么不能是8或者其他数字呢?”
无论是什么原因,在过去的40亿年左右,只有两种碱基对,即A-T、C-G,或者在RNA情况下的A-U,是大自然创造地球上无穷无尽生命所需要的一切基础。但论文通讯作者、佛罗里达州应用分子进化基金会项目负责人Steven Benner则表示,理论还有更多可能。
图:Steven Benner教授
当嘌呤(G或A)通过氢键与嘧啶(C、T或U)相连接时,碱基对就形成了。然而,也有其他嘌呤和嘧啶型的结构可以假设连接产生与标准DNA相同的螺旋结构。长期以来,科学家一直试图在遗传密码中添加更多对碱基。例如,在20世纪80年代,Steven Benner首次创造了“非自然”的碱基。其他研究小组也紧随其后。Steven Benner预计总共有4种其他氢键碱基对是可能存在的,它们由8个新的结构组成。他认为:“从本质上讲,DNA还没有完全利用其结构极限。正因为如此,DNA分子可以被扩展……你可以添加更多‘字母’。”
此前,Steven Benner研究团队已经将两个合成核苷酸(Z-P碱基对)结合到DNA中,并证明它们可以在体外复制和转录。现在,该团队再次增加了一种碱基对——S和B。
作为信息存储系统,DNA必须遵循可预测的规则。团队首先证明,与常规碱基类似,合成碱基能够可靠地形成配对。他们创造了数百个合成DNA分子,发现这些字母可以被预测地联系在一起。此外,研究团队还表明,无论合成碱基的顺序如何,双螺旋结构都能够保持稳定。该团队将化学合成的新型核苷酸整合到双链寡核苷酸(含有G、A、T、C、Z和P)中,然后测试了这些分子的熔解温度,即氢键断裂形成单链分子的温度。研究人员观察到熔解温度平均在预测值的2.1℃以内,与标准DNA寡核苷酸的误差范围类似,具可预测的热力学稳定性。三种不同“Hachimoji DNA”寡核苷酸的高分辨率晶体结构也证实了结构的相似性。
从化学上讲,“Hachimoji DNA”的外观和表现与标准DNA相似。然而,能够读懂和处理核酸的酶是很难被欺骗的,因此,为了将“Hachimoji DNA”转录成RNA,研究团队尝试了许多噬菌体RNA聚合酶变体,直到团队发现其中一种能够完成这项任务。利用这种RNA聚合酶,研究团队转录了一种已知的RNA适配体的“Hachimoji”版本。这种适配体名为“Spinach”,能够结合并照亮一个特定的荧光团。不出所料,转录的“Hachimoji RNA”能够如预期的那样发光。
毫无疑问,产生功能性“Hachimoji RNA”的能力为RNA生物技术领域开辟了许多可能性。RNA可以作为催化分子,所以使用新型核苷酸链,则可以产生更多官能团,它们可以与目标分子进行不同类型的相互作用,增加催化范围。“Hachimoji DNA”甚至可以与其他基于不同碱基对的人工合成核苷酸相结合,从而进一步提高功能。
对于这种刚刚问世的新型分子结构,无数更广阔的应用领域正在不远的未来。更重要的是,“Hachimoji DNA”的存在突破了自然界遗传语言的界限,或许在某个遥远的外星世界,生命形式正以我们从未想象到的形式存在。
参考资料:
1. S. Hoshika et al., “Hachimoji DNA and RNA: A genetic system with eight building blocks,” Science, 363:884–87, 2019.
2. DNA’s Coding Power Doubled
https://www.the-scientist.com/news-opinion/dnas-coding-power-doubled-65499
3. Four new DNA letters double life’s alphabet
https://www.nature.com/articles/d41586-019-00650-8
· END ·
Subscribe to:
Comments (Atom)